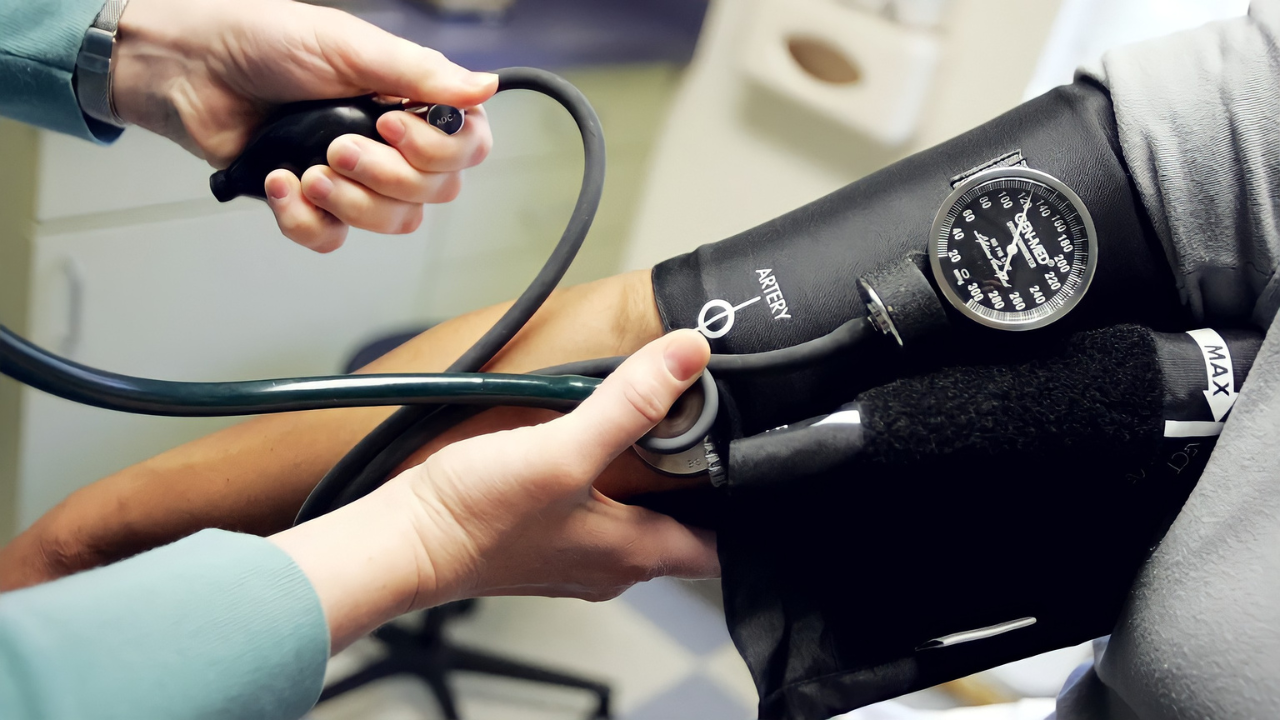
The Trump administration’s unprecedented decision to raise the H-1B visa fee to $100,000 for new applicants in September 2024 directly targets skilled foreign workers, including doctors, who comprise 25% of all American physicians. Approximately 50,000 India-trained doctors currently treat patients in the United States, making up a critical segment of immigrant physicians and supporting vital rural healthcare systems.
As a result of this policy, rural healthcare systems—already facing a shortage of native physicians—are now at greater risk of instability. Although the fee does not affect current visa holders, its impact on newcomers could accelerate the physician shortage projected to reach 124,000 by 2034.
The Historical Background of Immigrant Physicians’ Dependency on Rural Healthcare

Foreign-trained physicians who work in Health Professional Shortage Areas (HPSAs) are permitted to remain in the United States under the Conrad waiver program, which has been in place since the 1960s. The foundation of rural American healthcare for more than 60 years has been this pipeline, especially of Indian medical graduates, who have continuously filled gaps left by American-trained doctors.
This policy ethos has been drastically reversed with the $100,000 H-1B visa fee. Prior to the fee increase, foreign physicians kept hospitals from collapsing. For the first time, the cost of a visa for medical professionals is so high that it could reverse decades of advancements and worsen a health crisis in rural America.
The Policy Change of the Trump Administration and Its Direct Consequences

The decision to increase the visa fee to an unprecedented six-figure amount stands in stark contrast to the pressing need for medical personnel with foreign training. This policy was protested by more than fifty organizations, including the American Medical Association, which warned it would result in irreversible harm.
The fee essentially prevents new physicians from joining rural health systems, which are already experiencing a shortage. This risk is best illustrated by Dr. Mahesh Anantha’s practice in Batesville, Arkansas, where his cardiology services bring in over $40 million a year for the local hospital. However, the fee threatens to drive physicians like him out of the system completely. This fee is a financial death sentence for rural health, not just a bureaucratic obstacle.
The Extent and Severity of Physician Shortages
According to a UCSD study, there will be a 124,000 doctor shortage by 2034. This shortage already poses a threat to rural healthcare. In important states like California, Michigan, New Jersey, and Washington, DC, more than 30% of doctors are immigrants.
The reliance on foreign-born physicians is even more noticeable in rural areas. By preventing thousands of specialists and primary care physicians from entering, the $100,000 visa fee runs the risk of hastening the shortfall. For the estimated 15–20 million Americans who live in rural areas with inadequate access to healthcare, this policy upsets a delicate balance.
Economic Consequences for Rural Medical Facilities
Dr. Anantha’s $40 million yearly contribution to his Arkansas hospital is not unique; if one were to extrapolate this effect to all Indian-origin physicians, rural health systems would receive an annual economic boost of $2 billion. This revenue stream could be completely destroyed if visa fees are raised to $100,000. Hospitals, which are already overburdened, will find it difficult to find replacements or handle such an abrupt and significant cost increase.
These challenges could result in hospital closures, fewer services, and worse health outcomes for the local population because rural hospitals frequently operate on extremely thin margins. Communities that depend on these institutions will be impacted by the wider economic ramifications, which include job losses outside of the healthcare industry.
The Impact on Patients and Human Costs
The consequences are very personal for small-town America. The closest alternative facility is already a 1-2 hour drive away in places like Batesville, Arkansas, which has a population of about 11,000. Patients will no longer have access to near-home life-saving treatments if physicians like Dr. Anantha are priced out. This highlights a greater tragedy that may result in the loss of specialized medical care for about 1.24 million patients in rural America.
Vulnerable elderly, low-income, and chronically ill populations are disproportionately affected by the “death tax” imposed by the visa fee, which translates into longer travel times for urgent care, delayed diagnoses, and avoidable deaths.
Immigration Charges as a Risk to Public Health

Higher visa fees are frequently justified by conventional wisdom as safeguarding American jobs or generating income. This reasoning, however, is severely flawed in the medical field, where immigrant physicians fill an indispensable gap and domestic physicians largely avoid practicing in rural areas. More than it “protects” domestic jobs, fee increases disproportionately hinder foreign physicians.
Despite being politically presented as “protecting American workers,” this policy actually harms public health by making rural facilities more likely to fail and widening the gaps in healthcare across the country. The $100k fee may hasten employer closures and decrease the availability of medical services across the country rather than protecting jobs.
Cascading Impacts on the Workforce Pipeline and Medical Education

International medical graduates (IMGs) will probably be discouraged from applying for U.S. residencies as a result of the policy, which will reduce the pipeline that is essential for filling rural HPSAs. The closure of this pipeline exacerbates the shortage that medical schools are already experiencing due to capacity issues. IMGs offer language proficiency and cultural competency, which are crucial for a variety of patient populations, particularly in rural areas with high immigrant populations.
Fragile health environments may become even more unstable if current practitioners decide not to renew or relocate due to the fee hike’s chilling effect. Hospital closures, a decline in specializations, and an increase in care disparities are all consequences of this cascading workforce crisis.
Geopolitical Consequences and International Relations

About 50,000 doctors with training in India make up the largest group of foreign-trained physicians in the United States. The $100,000 fee runs the risk of damaging professional and diplomatic ties with India, a nation that has traditionally supported the exchange of medical education.
Talent may look for alternatives abroad as a result of this policy, which would restrict U.S. supply and jeopardize geopolitical goodwill. Furthermore, it might give other countries the confidence to erect reciprocal barriers, obstructing the international exchange of medical knowledge and innovation and further isolating the U.S. healthcare system abroad.
Source Data and Statistical Validation

The prevalence of immigrant labor in the healthcare industry is highlighted by the fact that one in four American doctors are trained abroad (AMA, 2024). For more than thirty years, the Conrad 30 waiver program has protected rural access by enabling foreign physicians with H-1B visas to work in HPSAs.
A clear timeline for the impending crisis is established by the UCSD 2024 study’s prediction of a 124,000 doctor shortage by 2034. Immigrants make up over 30% of doctors in populous states, demonstrating the nation’s reliance on these professionals. Therefore, the increase in the visa fee runs the risk of reversing these figures by discouraging new applicants and reducing the workforce at the exact moment when demand is at its highest.
Risk to Healthcare Infrastructure Increased by Fee Policy

Hospitals like the one in Batesville, which mainly depend on a small number of important doctors, serve as an example of the precarious infrastructure in rural America. The financial sustainability of these institutions frequently depends on experts with foreign training. Hiring such physicians becomes unaffordable due to the $100,000 fee, which puts facilities at risk of closing and specialized services being lost.
Reduced access to healthcare and economic downturns as hospitals close or reduce operations present a “double whammy” for rural communities. These issues deteriorate critical care and emergency services, endangering the rural health ecosystem as a whole and eroding public confidence.
Consequences for Community Health

The effects of the policy go beyond physical well-being. Psychological stress, anxiety, and a decline in community cohesion result from losing trusted physicians. In rural towns, patients develop enduring relationships with their healthcare providers; sudden losses exacerbate feelings of helplessness and anxiety. Uncertainty in healthcare can make substance abuse, mental health problems, and chronic illness management more difficult.
Senior citizens and low-income families are disproportionately affected by this hidden cost, which exacerbates a problem already made worse by rural isolation and socioeconomic difficulties. On several psychological levels, the $100,000 visa fee effectively jeopardizes community well-being.
Financial Stress on Families and Patients

Patients suffer direct financial harm outside of hospitals and systems. Longer care travel distances result in higher transportation costs, more time away from work, and more caregiving responsibilities. Treatment delays may result in more serious conditions that call for costly emergency procedures.
Families’ finances are impacted by the knock-on effects, which can result in higher debt, decreased income, and even poverty. This policy exacerbates healthcare disparities for already economically vulnerable rural populations, locking in cycles of poverty and poor health outcomes and ultimately driving up public health costs.
Possible Remedies and Alternative Policies
To stop or reverse this fee increase, immediate legislative action is required. Other options include increasing the number of slots in the Conrad program, offering targeted waivers for healthcare workers, or developing a tiered fee structure that acknowledges the importance of the healthcare workforce. Immigration adjustments must be accompanied by increased federal funding for rural health infrastructure and incentives for domestic rural practice.
Policies that prioritize interchangeability over obstacles will guarantee sustainable pipelines while enhancing equity. The United States runs the risk of widening disparities, expanding healthcare deserts, and negative economic effects in rural America if such measures are not taken.
The Existential Danger to Healthcare in Rural America

The $100,000 H-1B visa fee imposed by the Trump administration is a policy that will cause rural U.S. health systems to fail. It cuts off essential lifelines that foreign-trained physicians have been providing for decades, particularly in underprivileged communities, by erecting impassable financial barriers.
This policy exacerbates the anticipated shortage of 124,000 doctors, jeopardizes the financial stability of hospitals, puts 15–20 million rural patients at risk, causes financial losses, and exacerbates psychological distress. This fee has the potential to turn America’s healthcare crisis into a full-blown collapse with catastrophic repercussions that no community can afford if it is not removed right away or strategically mitigated.